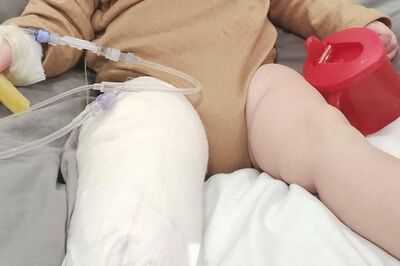
A mum has described how her baby daughter was left with lifelong disabilities after she raised concerns that were "ignored". Anna Martin said she contracted chickenpox while pregnant, which she claims doctors brushed off as "just a virus".
Anna, 31, said she attended her GP and A&E on five separate occasions, but claims her worries were consistently dismissed and she never received treatment for the illness despite clear warning signs. This had catastrophic results and Anna suffered a serious complication, which meant her daughter Genevieve was born in November 2022 with congenital varicella syndrome - an uncommon and serious condition.
She was also born with longitudinal limb deficiency and fibular hemimelia, meaning she has a shortened right leg and three toes on her smaller foot. Anna and her fiancé, Iain Lewis, 32, took the heartbreaking decision to amputate her right foot when she was just 14 months old.
- Foreign Office updates advice for seven Middle East countries for stranded Brits
- 'I’m a GP - I changed these things in my home to reduce cancer risk'
Genevieve, now three, also faces a heightened risk of multiple learning difficulties, secondary sight and hearing loss, as well as limb deformities. Anna has now initiated legal proceedings against Chesterfield Royal Hospital in Derbyshire and her surgery and is urging the NHS to safeguard pregnant women.
Secondary school teacher Anna, of Chesterfield, said: "What should have been a normal, joyful pregnancy became a nightmare because of a preventable failure in the system. We were let down by the NHS, by my GP surgery and by Chesterfield Royal Hospital.
"Most of all, we were let down by a policy that values assumption over simple testing - a policy that continues to put pregnant women and their babies at risk."
At just five weeks pregnant, Anna's daughter, Josephine, five, returned home from her childminder with chickenpox. Anna quickly fell seriously unwell with fever and flu-like symptoms and visited her surgery explaining she had been exposed – but claims she was repeatedly told it was "just a virus" and no test was offered.
Anna added: "I went to my GP and was asked whether I'd had chickenpox as a child. I explained that I wasn't sure; my mum thought I probably had, but there was no certainty. I was told it was likely a virus and sent home.
"Over the next week, I returned to the GP twice more as my symptoms didn't improve and my fever wouldn't settle. Each time, I was reassured that it was a virus and sent home again.
"The next day, I noticed a painful spot behind my ear and went straight to the hospital. I was isolated in a side room and told it looked like chickenpox, but staff were unsure how to proceed.
"I was left for several hours without care. I was then transferred to the Women's Health Unit, which had actually closed shortly before my arrival.
"I was left waiting in a corridor with a locum healthcare assistant before being reluctantly allowed inside and I was repeatedly told I shouldn't have been brought there as I was a risk to other pregnant women. I was swabbed and sent home to wait for a call from an obstetrician. When no one contacted me the next morning, I rang myself for guidance.
"Despite explaining how unwell and frightened I felt, I was advised to stay at home. I was told I could return to A&E if I felt I couldn't cope, which I did. I was then admitted to the Emergency Medical Unit, where I was largely isolated, not allowed visitors and left without access to basic washing facilities."
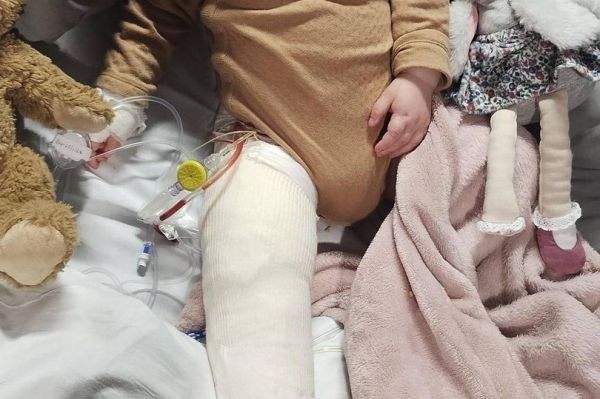
GPs were adhering to current NHS guidelines – whereby adults are only offered a blood test to check for chickenpox antibodies if they are completely certain they have never previously contracted the virus.
Anna went on to say: "Many pregnant women, like myself, are unsure of their chickenpox status and are left at risk when exposed to the virus. This is a massive flaw in the system – and one that cost my daughter dearly.
"If I had been offered that simple blood test at my first GP visit - or even my third - my infection could have been recognised in time. Antiviral treatment could have been started earlier and the condition could have potentially been prevented.
"Instead of being listened to or helped, I was refused treatment. I was left alone in a side room for hours.
"Eventually I was transferred to the Women's Health Unit, who didn't want to see me, telling me I was a risk to others. They reluctantly swabbed my rash, but still gave me no treatment and sent me home. It wasn't until the following evening, after I took myself back to AandE again, that I was finally given antiviral medication."
Yet by the time chickenpox was finally identified, the damage had already been done.
She continued: "Something I find baffling when you consider that chickenpox is not a virus we test for in order to diagnose and the amount of adults now who would have clinical proof of the childhood illness is very rare. Instead, it was presumed I had it and therefore I was not tested until two weeks after showing symptoms and far too late to make a difference to my daughter contracting the illness.
"She is currently doing well. She suffers with fatigue and pain/spasms most nights, but she is mobile in moderation and full of light and laughter."
Anna has lodged a formal complaint and medical negligence claim against both the hospital and health centre. She has also set up a petition on Change.org urging the NHS to review its current policy to automatically screen pregnant women for chickenpox antibodies whenever exposure is suspected, regardless of whether they believe they contracted chickenpox during childhood.

She added: "What matters most to us, as parents, is raising awareness of how dangerous chickenpox can be in pregnancy and highlighting a clear gap in current NHS guidance. At present, NHS guidance recommends testing vulnerable adults exposed to chickenpox only if they are certain they have never had it before.
"As a mother, I find this deeply worrying. Many of us were never tested as children, and diagnoses were often based on memory or visual assessment alone. It is also possible to contract chickenpox more than once.
"We believe that pregnant women - particularly in early pregnancy - should be offered antiviral treatment while blood tests are being carried out, regardless of uncertainty about past infection. Antivirals are considered safe in pregnancy and could prevent babies from being exposed to Congenital Varicella Syndrome.
"Had a more preventative approach been taken, my daughter may have been spared the disabilities she now lives with. While we are positive and hopeful about her future, we are also very aware that this could potentially have been avoided. Our intention is not to place blame, but to help protect other families from going through the same heartbreak."
Krishna Kallianpur, chief nurse at Chesterfield Royal Hospital, said: "We continue to work with representatives of Ms Martin in respect of the care of her daughter, and the concerns she has raised with us. As the investigation and legal process continues it would be inappropriate to make further comment."
-
The Phones Of Tomorrow: 5 Wildest Concept Devices Showcased At MWC 2026

-
IIT Madras PG Diploma In Manufacturing Analytics Registrations Underway; Check Eligibility Criteria, Application Process And Fee Structure
-
Arjun Tendulkar-Saaniya Chandhok Wedding: Shah Rukh Khan, The Bachchans, Farhan Akhtar & Other Celebs Attend Sachin Tendulkar's Son's Marriage

-
Government of India Hiring Aadhaar Operator Supervisors Nationwide

-
Government of India Hiring Aadhaar Operator Supervisors Nationwide
